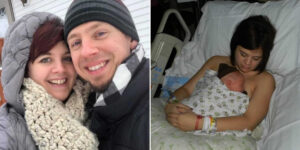
I always imagined having four children. I don’t know exactly why—it just felt right. In December 2006, thirteen months after Jeff and I got married, we lost our first baby. The devastation was overwhelming. Months of negative pregnancy tests followed, each one a heartbreak in itself, until our rainbow baby finally arrived. Our daughter, Presley, was born in 2008, followed by our son, Dax, in 2010. Even as the years passed, I still longed for that fourth child. Jeff, like most husbands, worried about finances, so it took time before we tried again.

When we discovered we were expecting in late 2016, the excitement was electric! Since we already had a boy and a girl, we decided to wait until the birth to find out the gender. The suspense made the pregnancy thrilling. Aside from the usual morning sickness, everything seemed perfect. But in the final weeks, I noticed less movement. Fearful of repeating history, I visited labor and delivery multiple times. Each time, I was hooked up to the Doppler, heard the heartbeat, and was sent home reassured. Even at one of my last weekly checkups, my doctor ordered a Doppler due to reduced fetal movement—again, everything seemed fine, until the big day.
August 22, 2017, was supposed to be magical. We arrived at the hospital ready for our gender reveal surprise, but reality had other plans. Before surgery, I had filled out paperwork to donate my placenta to a program helping burn victims. It felt like such a meaningful way to give back. Riding high with excitement, we went into the O.R., only to have our joy shatter the moment Dallas was born. There was no cry—just a tiny squeak. Dr. M said, “It’s a girl,” handed her to the nurses, and left.
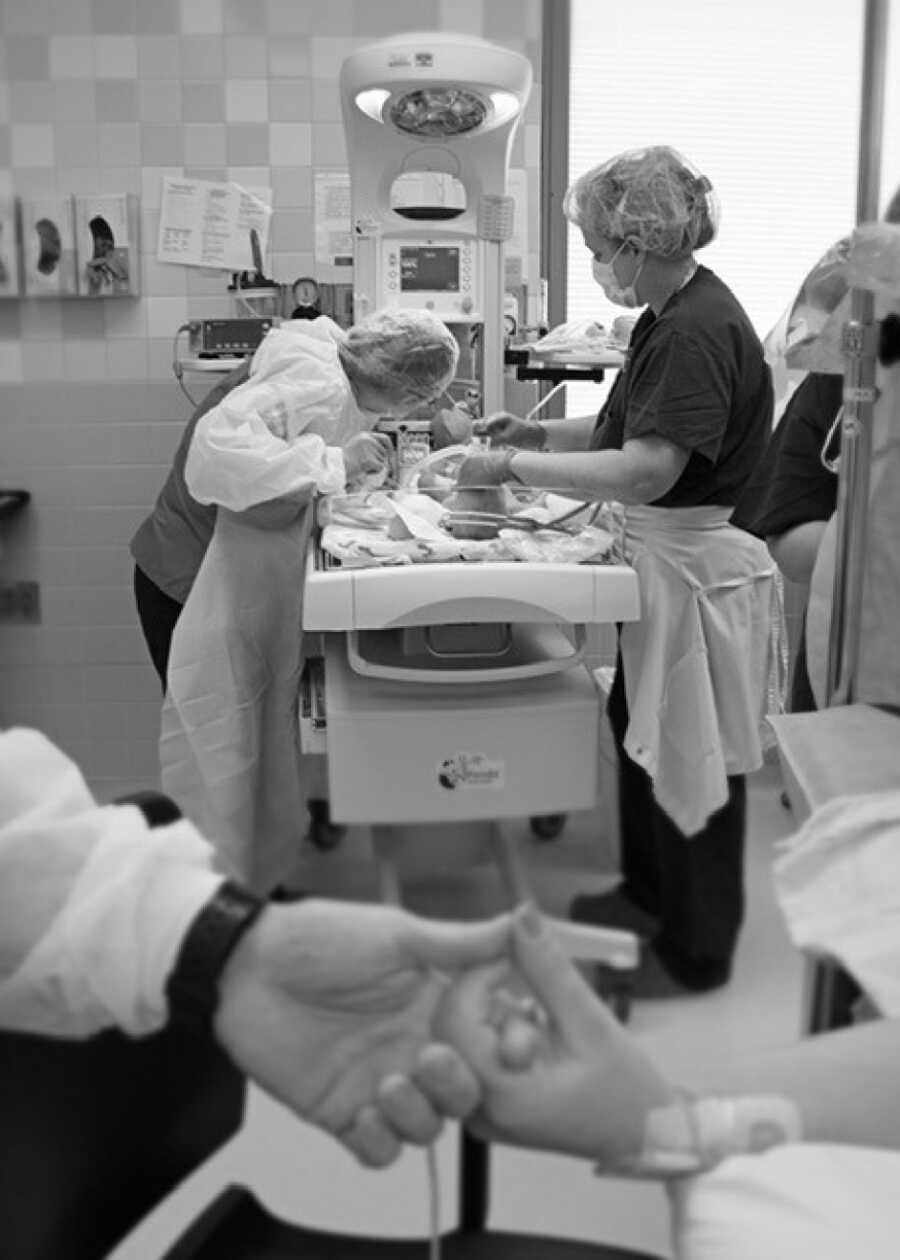
Something was terribly wrong. I begged Jeff, “Don’t leave her. Please don’t leave her.” Nurses continued bagging her with oxygen as I frantically asked what was happening. Her lungs were sticky, and she needed immediate care in the NICU. Soon, we learned our daughter, Dallas Jane Parker, was critically ill—born full-term but with a collapsed lung, a premature collapsed lung, a raised right diaphragm, and severe pulmonary hypertension. She was intubated, given a chest tube, and placed on an oscillating ventilator. The doctors told us she might not survive.
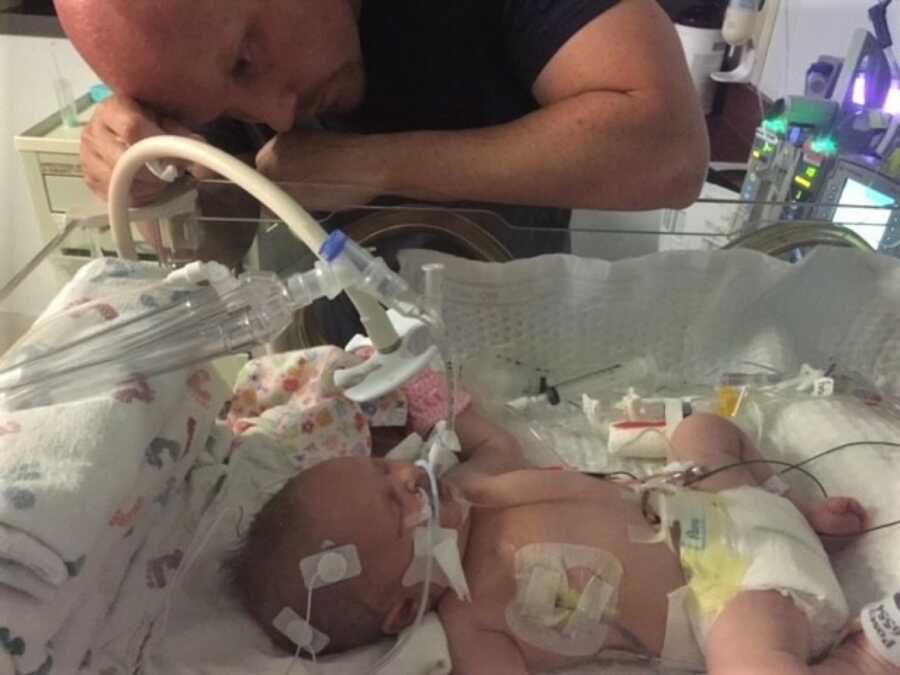
I didn’t cry—I was furious. “You are known for your NICU! Women come here for your expertise. Don’t tell me you’ve done all you can. Figure it out!” We had a clergyman come to baptize her in the NICU, in case the worst happened. The doctors explained that her only chance, as slim as it was, would be ECMO—heart and lung bypass. A machine had just become available at another hospital. It was risky to transport her, but staying meant certain death. Jeff left with Dallas, and I stayed behind, stunned, learning my placenta donation wouldn’t work either—part of it had calcified with Dallas inside.
At Medical City Children’s Hospital Dallas, Jeff was told she had made it alive, but she still faced a life-or-death fight. ECMO was a huge feat, and I couldn’t bear being away. I had seen her face and touched her skin only a few times. My baby was on death’s doorstep, and if she was going to leave this world, I wanted her to know she was loved. With the support of my dear friend Kim, and understanding from my OB, I left the hospital about 24 hours after my C-section to be with her. Seeing her hooked up to cannulas and lines was heartbreaking, but I had to focus on the fight ahead.

Day six and a half brought hope—her pulmonary hypertension resolved, and we could trial coming off ECMO. Ecstatic, we walked in the next morning to chaos: Dallas was bleeding internally and had a blood clot in her cannula. Minutes from death, we said our goodbyes and begged her to stay. I pumped milk through tears, not knowing if she would live to eat it. Our warrior girl survived all three emergency procedures.
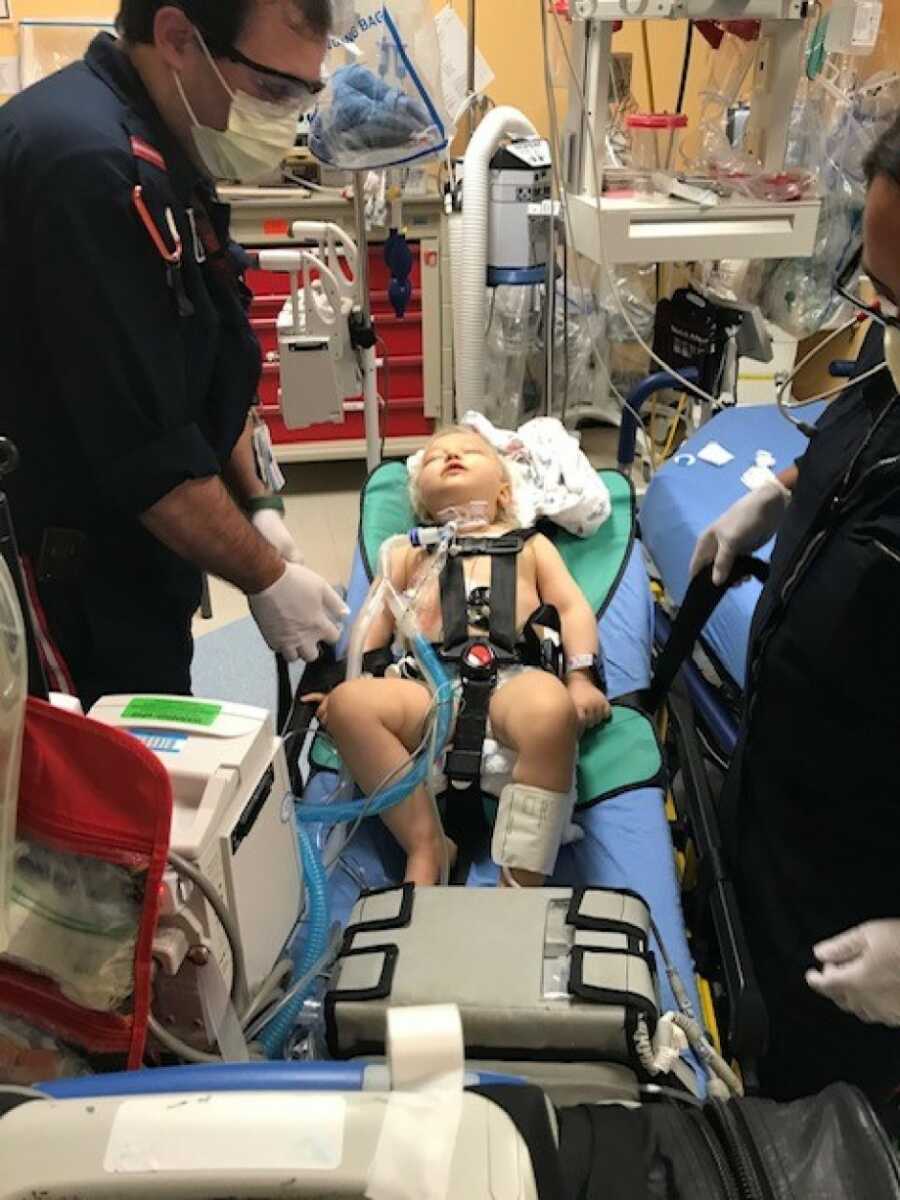
One week later, we were dropping the older kids off at school when the hospital called—Dallas had coded and required CPR. Traffic made the journey an hour and a half. She developed systemic capillary leak syndrome, doubling in fluid weight overnight. Swollen, sedated, with skin splitting, our tiny fighter looked like she’d been through a battle. At 23 days old, she was finally stable enough for us to hold her—a process that took five people over thirty minutes.

Her challenges continued: recurrent chylothorax, multiple chest tubes, tracheostomy, G-tube, nearly six months inpatient, and then finally, home. Tracheostomy was terrifying but the best decision for her independence, allowing mobility, speech, and freedom. Her seizures, severe and unpredictable, often leave her oxygen-deprived and blue. She faces a high risk of SUDEP, yet we persist. Our older kids help care for her during emergencies, literally breathing life back into their sister. They are heroes beyond their years.
Isolation has been another challenge. I left my career to care for Dallas, becoming nurse, PT, OT, advocate, scheduler, and more. Socially, life shrank—friends drifted, and our outings are limited for safety. Support from other parents in similar situations has been a lifeline. Dallas has spent half of her four years in hospitals, yet she continues to defy odds. She faces every obstacle with courage, collecting rare diagnoses like trophies. She is our unicorn, our miracle, and the perfect final piece of the Parker puzzle.

Dallas Jane Parker turns four this August. Despite seizures, chronic illnesses, and countless medical hurdles, she is the feistiest, most resilient little girl we know. She teaches our family about strength, compassion, and hope daily. We will never give up. We will always advocate. She is living proof that miracles come in the form of fighters—and she continues to inspire everyone lucky enough to meet her. Dallas Jane Parker arrived full-term and full of surprises, and she is thriving every day by living that motto.