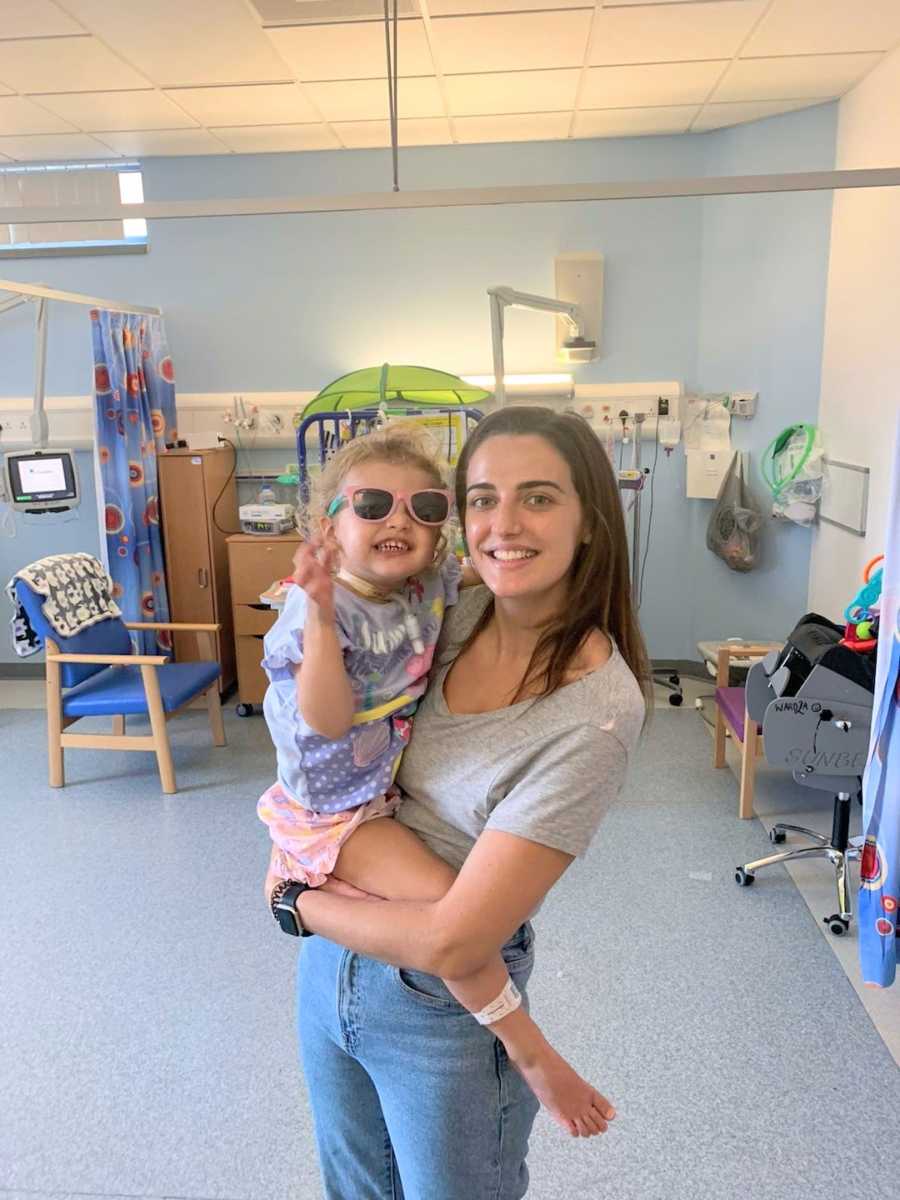Going for my 20-week scan, I wasn’t expecting any surprises. We had decided to keep the gender of our baby a secret, so I walked into that appointment thinking it would be a normal, joyful check-in. But when I walked out clutching my case notes, my eyes fell on four words that made my stomach drop: “Abnormal Heart Vessels.” The scan itself became a blur. My partner and I just stared at each other in disbelief and whispered, “What the hell just happened?”—both of us lost and unsure of what to feel.
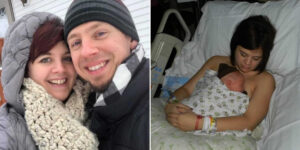
The following days stretched on like an endless nightmare. After meeting with two fetal heart specialists, we finally had a diagnosis: our baby had a congenital heart defect called a right-sided aortic arch. They reassured us that, despite the unusual growth of her heart vessels, her heart itself would work perfectly. Monthly scans showed her growing beautifully, and for a while, we allowed ourselves to breathe, believing she was healthy. When I gave birth to our baby girl, Elodie, joy completely overtook me. The instant connection I felt was overwhelming—a love so deep I didn’t know existed.

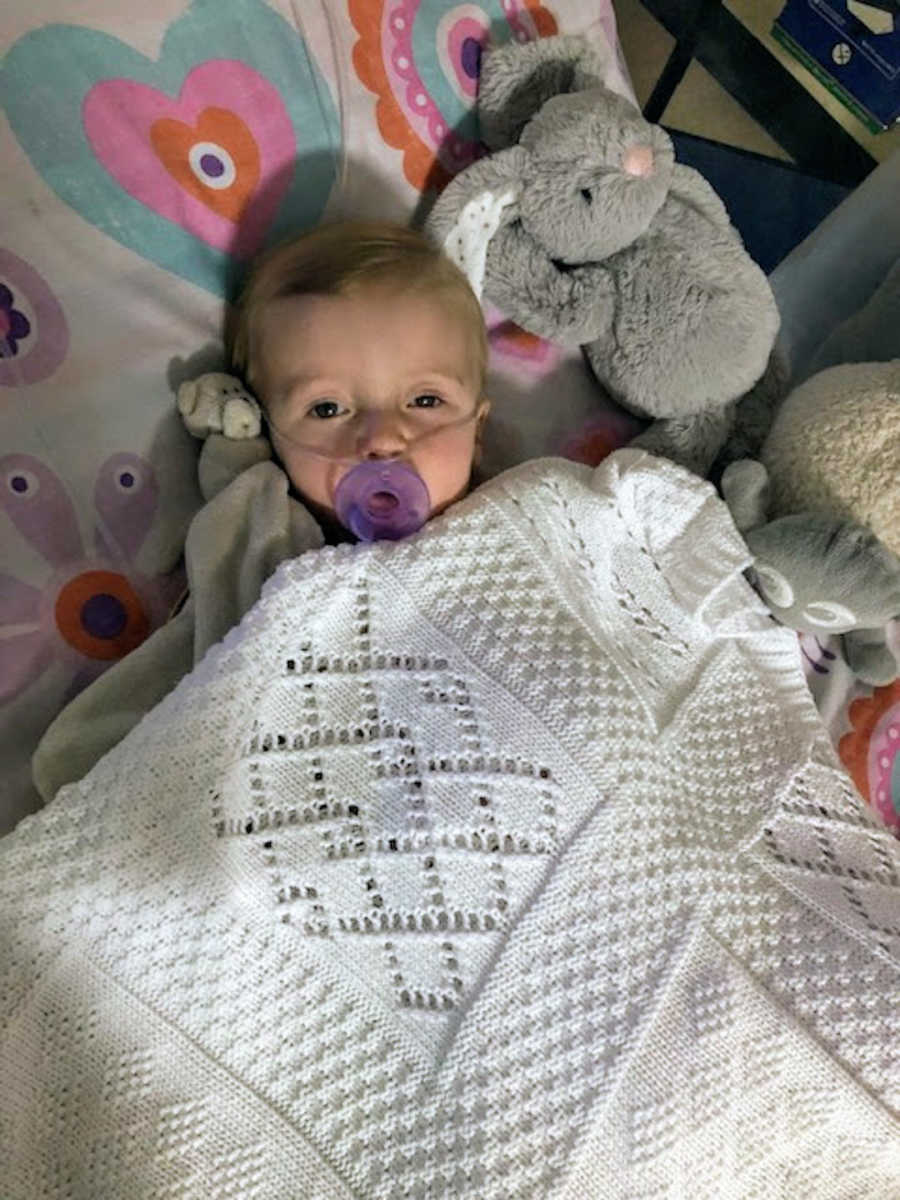
At six months old, when we started introducing solid foods, I handed Elodie a small rice cake. After a few bites, she turned blue at the lips. It was every parent’s worst nightmare. What terrified me even more was that these episodes became frequent. Friends, family, and even our health visitor reassured me it was probably just a sensitive gag reflex. But my instincts screamed that this wasn’t normal. I returned to her consultants to explain what had happened, expecting a dismissive response—but instead, they were concerned.
Elodie underwent a CT scan and a barium swallow, which confirmed she had a vascular ring—her heart vessels were compressing both her esophagus and trachea. At just one year old, she faced her first heart surgery. Looking back now, it seems manageable, but at the time, it was devastating. Laying your baby on a surgeon’s table is a reality no parent should ever face. Miraculously, Elodie recovered quickly and was discharged in three days. Going home felt like life had returned to normal, and for a short while, we allowed ourselves to hope that the worst was behind us.

Three months later, the blue episodes returned, more intense and frightening than before. Another CT scan and barium swallow revealed the vascular ring had recurred, compressing her esophagus again. My devastation was total. The congenital heart defect we had been told was “not serious” had become a life-altering reality. The fear of what was next—and whether it would even be fixable—was unbearable.
We returned to the cardiologist, who explained that Elodie’s only solution was major open-heart surgery: a complex procedure to reimplant her aortic arch correctly. Hearing the surgeon outline the options—do nothing (potentially life-threatening), live with a PEG tube for life, or undergo surgery—made my stomach turn. This was my baby. My daughter. I could hardly breathe as I processed the gravity of what he was saying.
After long discussions, my partner and I knew the right path was surgery. We naively hoped recovery would be smooth and short, like her first operation. Elodie went under the knife, and after seven hours, the call came: the surgery was a success. But moments later, as they attempted to remove her from the ventilator, it became clear something was wrong.
Medical staff rushed around her as she struggled to breathe, her tiny body working so hard it was visible in the movement of her chest. I pleaded for them to put her back on the ventilator, and thankfully, they agreed. Alone in the PICU due to COVID restrictions, I sat beside her in full PPE, desperately searching for reassurance in the eyes of nurses who couldn’t give me any. I couldn’t believe this was real. I blamed myself, thinking, I led her here. This is my fault.
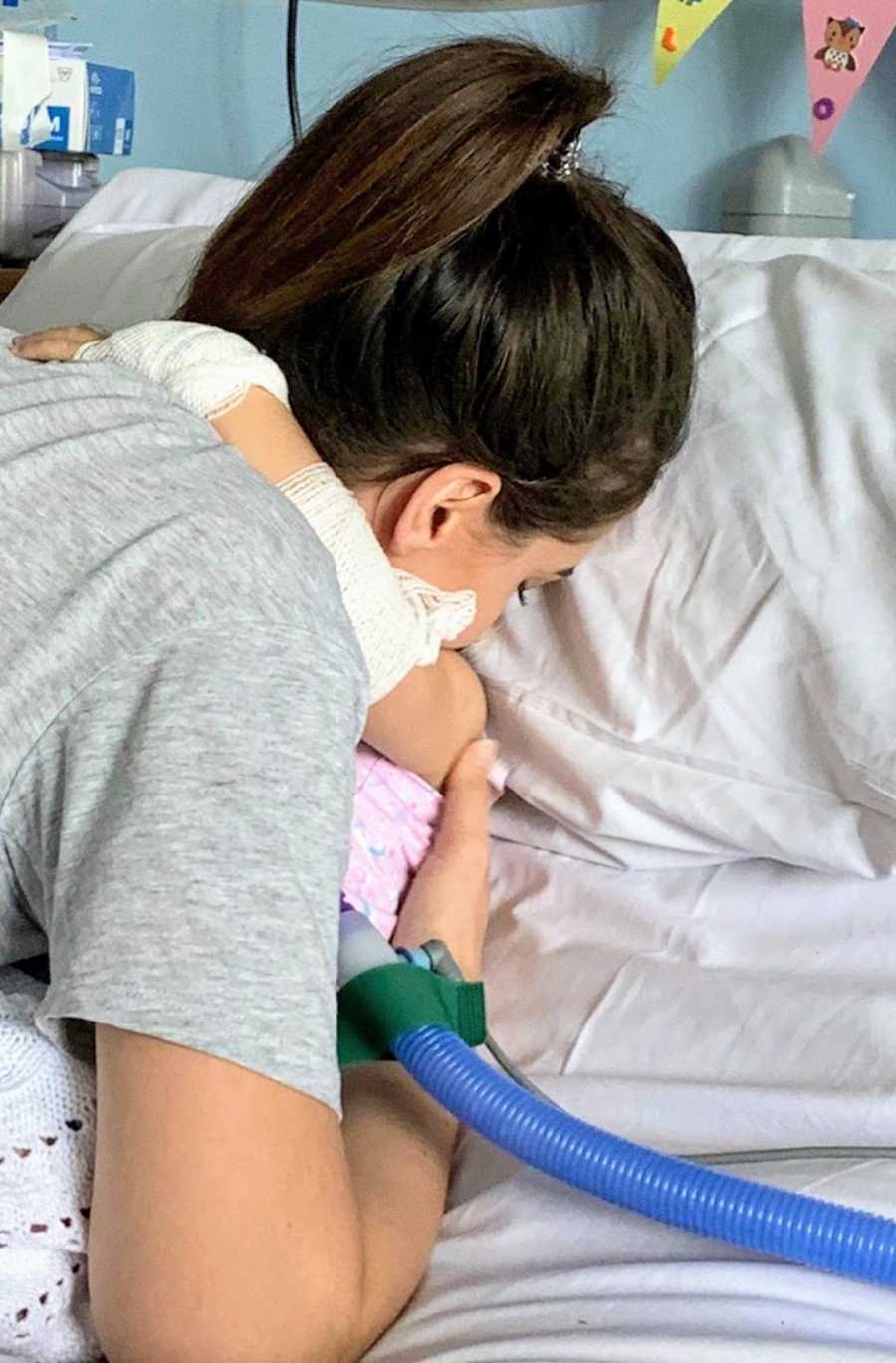
A PICU consultant informed me that Elodie needed another procedure—a bronchoscopy. I was terrified. She’s too weak, I thought. The consultant understood but insisted it was necessary. I cried, asking, “Promise me she’s going to be okay.” Her reply, “We’re really concerned,” shattered me. I called my sister, hysterical, convinced I might not take my daughter home.
Before her bronchoscopy, I sat with an ENT specialist and a respiratory consultant. All I could ask was, “Am I going to get my Elodie back?” Their cautious optimism—that long-term, she would recover—was both comforting and terrifying. During the procedure, it became clear her airways were collapsing due to the persistent pressure from her heart vessels.
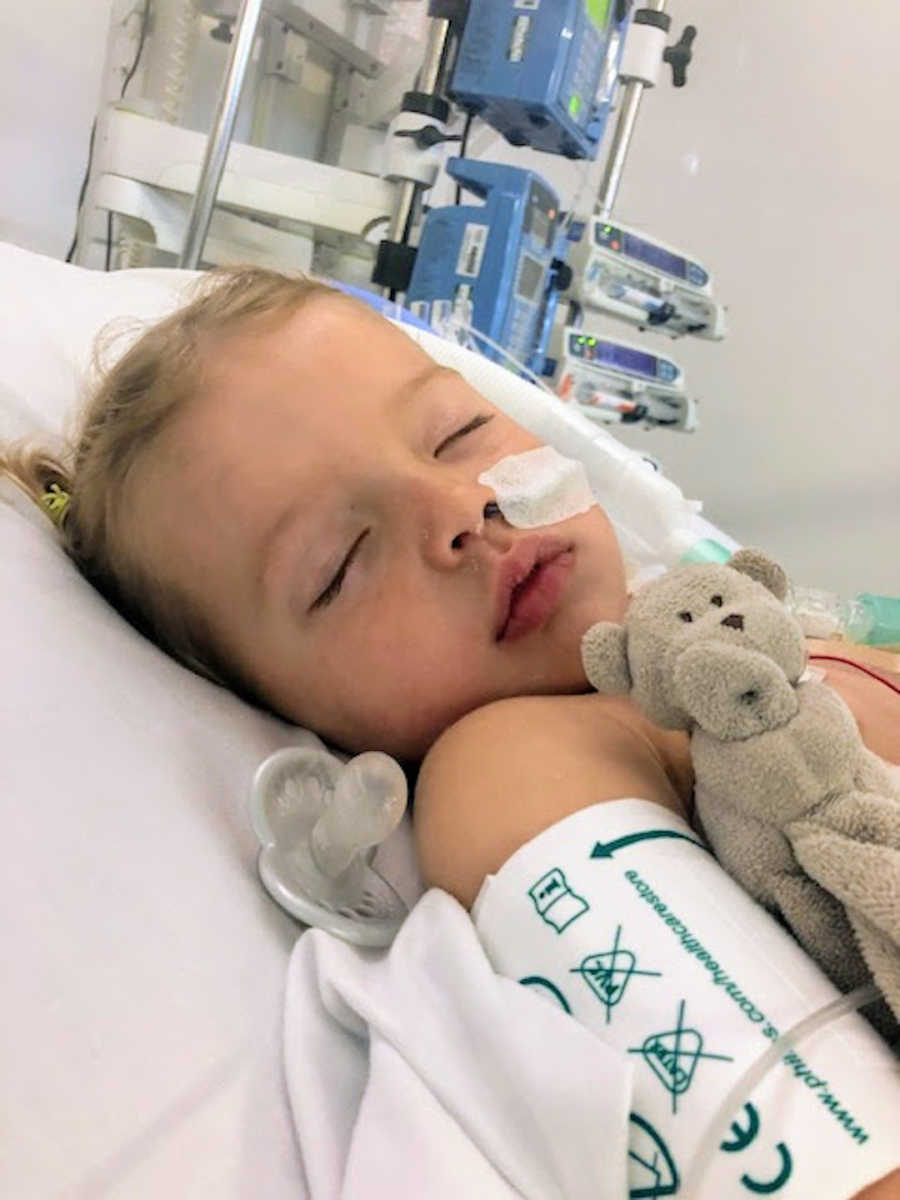
Elodie spent ten days heavily sedated on a ventilator in the ICU. Each day brought new terrors: periods where she had to be resuscitated, phone calls in the night informing us her oxygen levels had dropped. Those were the darkest days of my life. I couldn’t fathom how my two-year-old needed life support to breathe. Anger, fear, and despair consumed me.
Her final airway assessment revealed severe tracheomalacia and bronchomalacia—the lifelong damage caused by her previously compressed airways. Even though her heart was fixed, the consequences were devastating. The only solution: a tracheostomy and ventilator. My first reaction was devastation; my second was relief. Relief that something could be done to save her life.
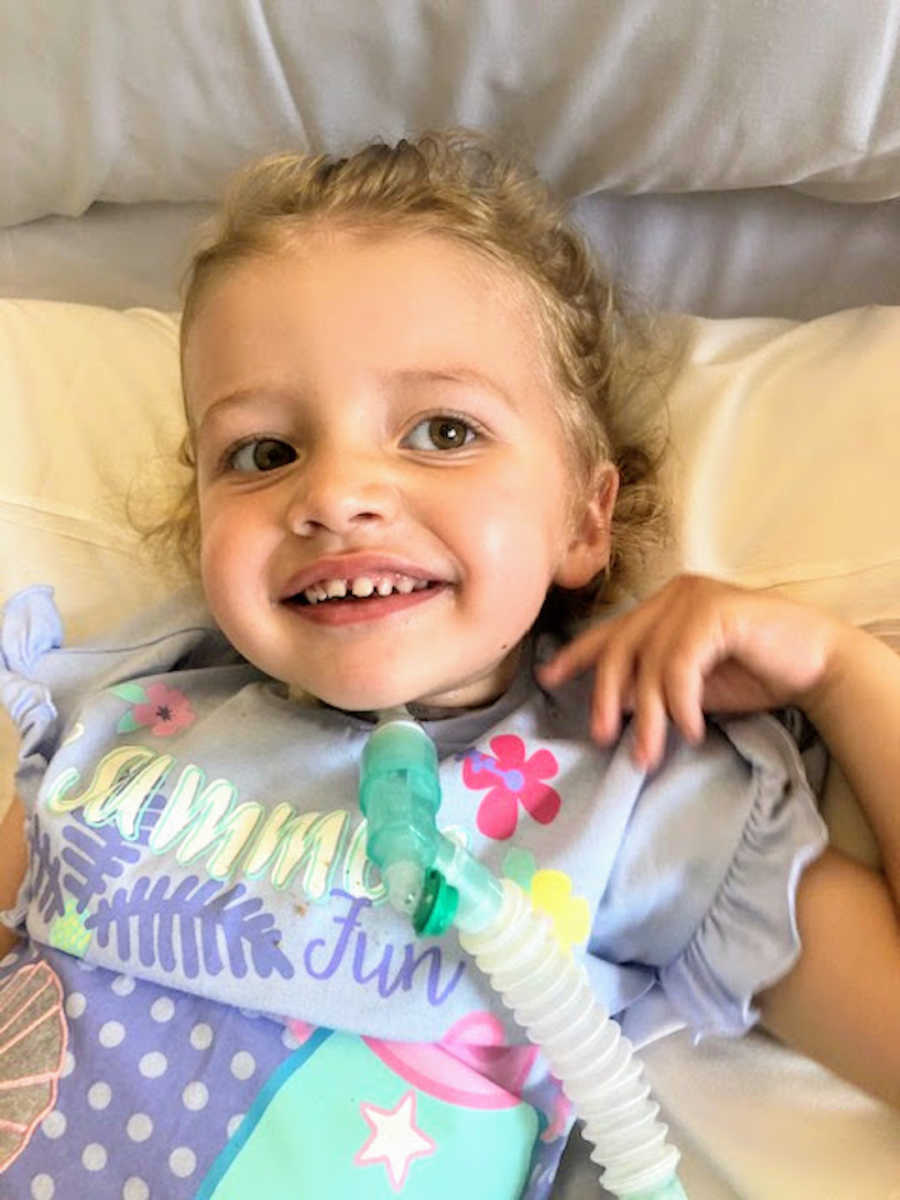
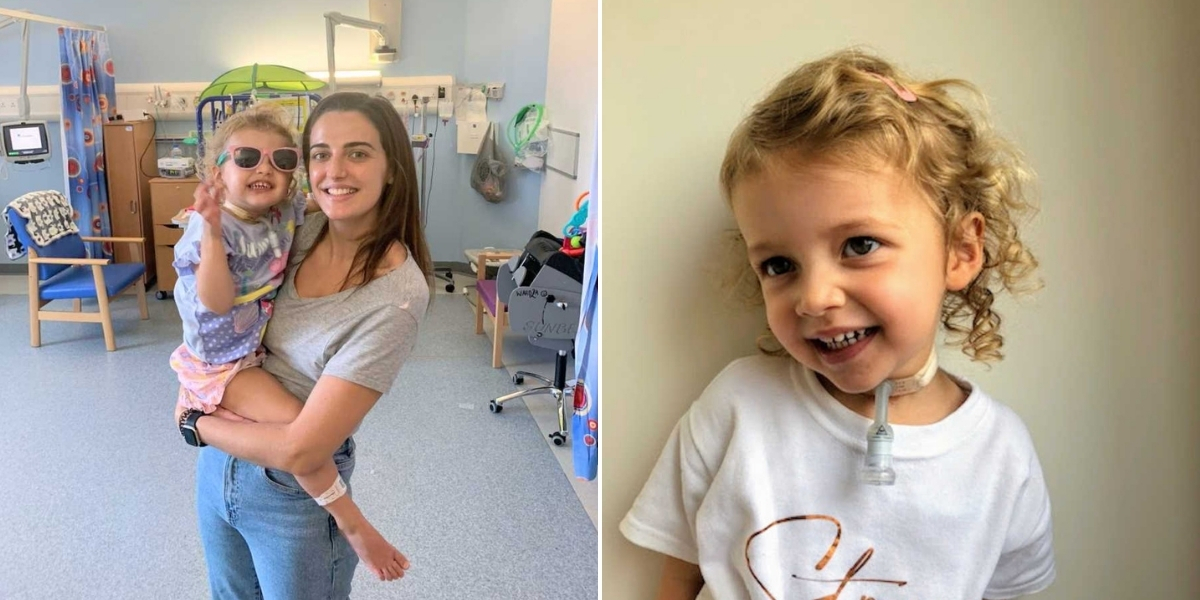
Despite everything, Elodie remained a vibrant, happy, and intelligent child. Seeing her face with the tracheostomy was heartbreaking but also a relief—she was finally able to breathe properly. The nurses and doctors celebrated her progress, and day by day, we saw more of the little girl we knew. The recovery was long and challenging; she had to relearn how to walk, talk, and eat. Over time, one of her airways improved, and she began breathing without the ventilator, able to speak through a valve. Six months into life with a tracheostomy, the journey is still emotional, but each milestone feels miraculous.

We have experienced unimaginable lows, but equally profound highs. Bringing her home after two months in hospital remains the happiest moment of my life. I wish I could tell any parent facing such a path that things will be okay. I am eternally grateful for the small tube in her neck—it literally saved her life.
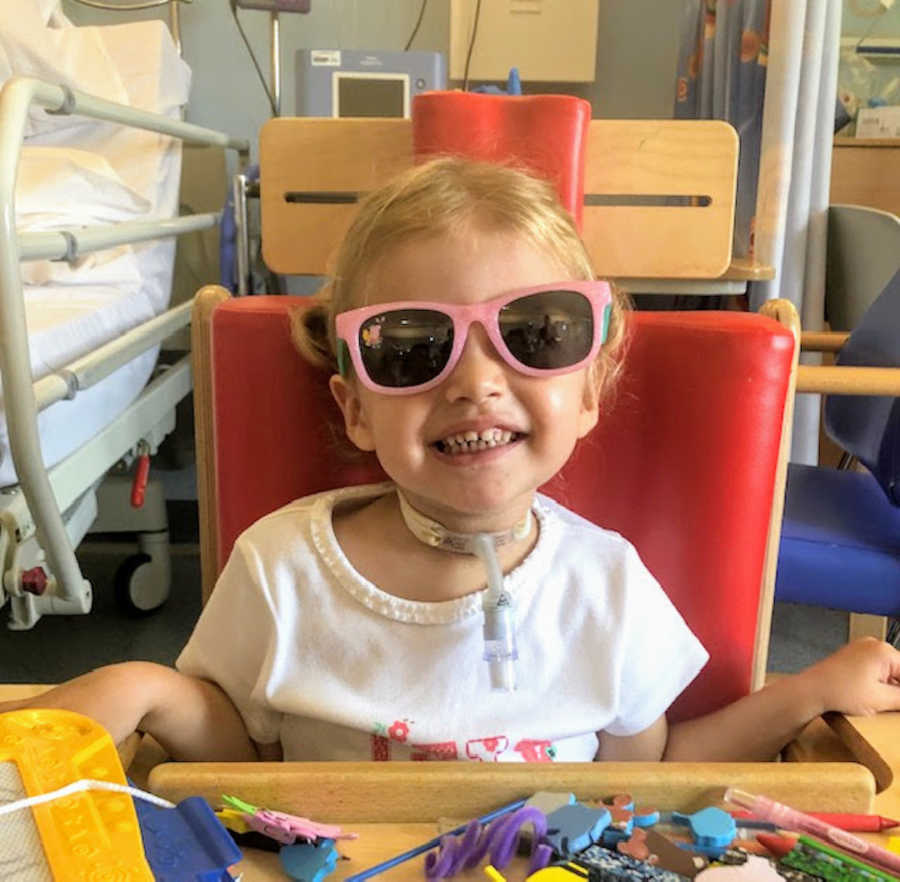
Elodie is now an inspiration to everyone who meets her. She has embraced her tracheostomy fully, living her life without letting it define her. Each day, we see her thriving, and every glance at her fills me with pride. Consultants are confident that, as she grows, her airways will strengthen and eventually allow her to have the tracheostomy removed.

I don’t see Elodie as disabled. I see my brave daughter, resilient and unstoppable. My fears that she wouldn’t be the same have vanished. After everything we’ve been through, life feels profoundly precious. I will never take small moments for granted again. I love Elodie more than I ever thought possible, and every day, she makes me proud beyond words.