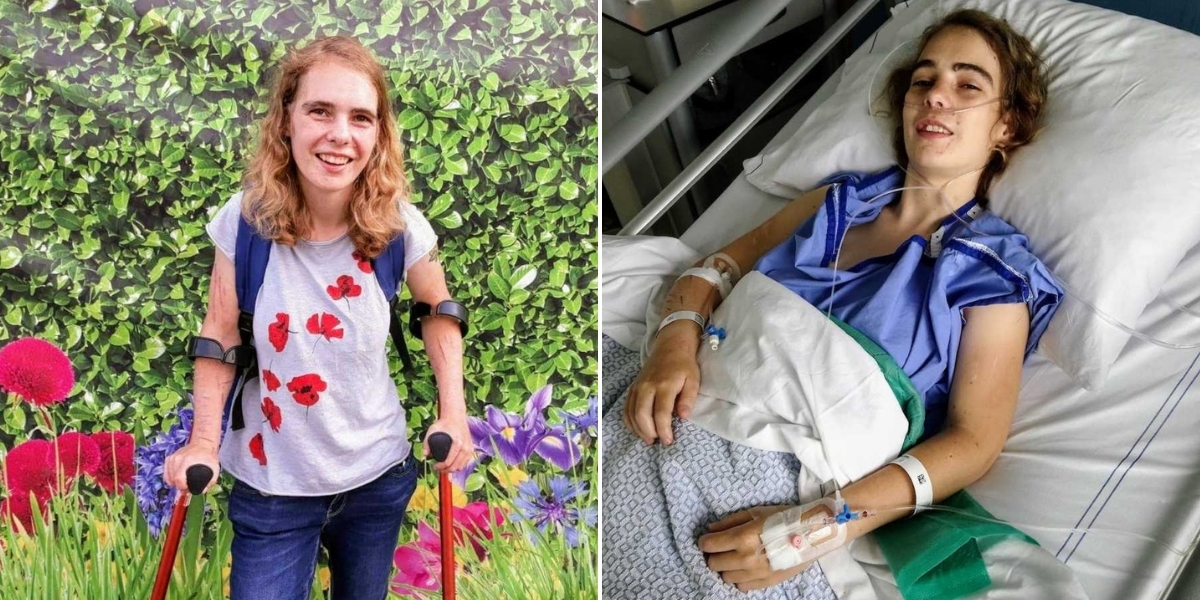
I grew up in a small village in the Netherlands called Oosternijkerk. It was the kind of place where everyone knew one another, shared their own language, belonged to the same circles of friends, and supported the same soccer club. Yet somehow, I never truly belonged. I didn’t fit in there, and I didn’t fit in at school either. From a young age, I knew I was different. My bones were different. I couldn’t walk straight, and I couldn’t sit or stand for long periods of time. My mobility wasn’t like that of other children, and no one knew why. There were no answers, only questions.
When I was three years old, my mother noticed something unusual. She felt what seemed like extra bones and feared I might have fractures. That concern led us to an orthopedic specialist. Even then, doctors couldn’t identify the cause. There was no diagnosis and no treatment, only medication to manage symptoms. I have two younger brothers, now 25 and 19, and my youngest brother was later found to have the same bone disease. By the time I was 12, my condition worsened to the point where I could no longer walk properly. My legs had grown into an X-position, making surgery unavoidable. I underwent an X-leg correction just to be able to move again.

During my adolescence, the pain intensified. It spread everywhere throughout my body, and my brother experienced the same thing. That’s when it became clear the condition was hereditary. Our general practitioner did further research and finally discovered the name of this rare disease: MHE-MO, or Multiple Hereditary Exostoses—Multiple Osteochondromas. Before we had a name, it was almost impossible to explain what was happening to me. Having a diagnosis changed everything. It led us to a support group, and for the first time, we realized we were not alone. We met people my age and others my brother’s age. The youth days were the highlight for me, and the workshops taught us so much.
MHE-MO affects the long bones of the arms and legs, as well as the pelvis, ribs, and shoulder blades. The disease is characterized by multiple benign bone tumors, known as exostoses or osteochondromas. It is a hereditary congenital condition with an autosomal dominant inheritance pattern, meaning only one mutated gene is needed to be born with the disease. This also means there is a 50% chance of passing it on to your children. My brother and I inherited it from our mother, who inherited it from her mother, and so on through generations. MHE-MO is caused by mutations in either the EXT1 or EXT2 genes on chromosomes 8 and 11. It is rare, affecting about 1 in 50,000 people. In the Netherlands alone, around 1,000 individuals live with this disease.

Because of a missing signal in my chromosomes, parts of my bones never stopped growing. Extra bones formed near my joints, causing serious complications. Some of these exostoses pressed against nerves, muscles, and blood vessels, resulting in severe pain. Surgery is the only way to relieve that pressure and reduce danger. I have undergone 15 surgeries so far. It feels like a lot, though I know others have endured even more.
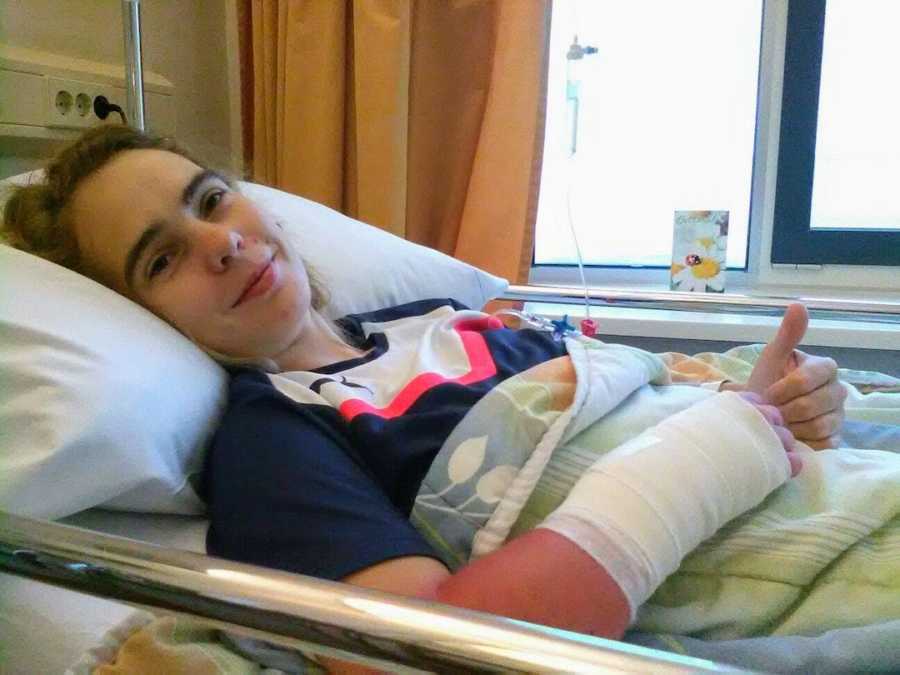
People with MHE-MO must have MRIs every one to two years because there is a risk that the exostoses can turn into bone cancer. Thankfully, that has not happened to me yet. Still, living with MHE-MO is incredibly demanding. It comes with chronic joint pain, countless surgeries, pain treatments, physiotherapy, and occupational therapy. There is also a 10% risk of developing bone cancer and a high prevalence of mental health struggles. Research is ongoing to find medications for children that could prevent deformities and stop exostoses from forming, potentially eliminating the need for surgeries in future generations.

School and work were always a struggle for me. Chronic pain affected my concentration, and I missed many classes due to hospital visits, pain treatments, and surgeries. At times, I spent three days a week in the hospital in Amsterdam. Recovery after surgery officially takes six weeks, but in reality, it often takes much longer. One surgery failed, leaving me with permanent nerve damage in my left leg. Later, I developed CRPS—Complex Regional Pain Syndrome. My pain system became disrupted, and there is no cure, only pain management. I have CRPS type two, which includes nerve damage. My symptoms include reduced blood flow, temperature differences in my legs, hypersensitivity to touch, sweating, and the inability to feel the ground beneath my feet.

CRPS is sometimes called “the killing disease” because of the unbearable pain it causes daily. I go to bed in pain and wake up with even more. Both CRPS and MHE-MO completely changed my life. My treatments include medications such as Lyrica, naproxen, amitriptyline, and fentanyl—stronger than morphine—as well as nerve blockers, lidocaine injections, and ketamine infusions three times a month. Ketamine is extremely heavy on both the body and the mind.
My very first surgery, the X-leg correction, was traumatic. The drain in my leg was placed incorrectly, causing severe bleeding that wouldn’t stop. I lost a lot of blood, and my father fainted in front of me. I was only 12 years old, lying in a bed covered in blood. I was in shock for three days. That experience, combined with later medical trauma, resulted in PTSD, along with a severe fear of needles and blood.
From that point on, life felt like a constant struggle. I was bullied at school because I needed crutches, couldn’t participate in gym class, and struggled during lessons involving blood. I became shy, insecure, and emotionally closed off. I didn’t talk about my feelings at home or at school. Instead, I buried them so deeply that I felt empty. I felt misunderstood by everyone—my parents, friends, doctors, and teachers. I carried my pain alone, especially during quiet moments, bus rides, and school breaks. I had nightmares about blood and surgery and struggled to sleep, but I thought it was normal and never spoke about it.

As I got older, I tried to feel nothing at all. I drank heavily on weekends. At 19, I was raped by my uncle’s best friend in my uncle’s house. He had known me since I was a baby, and I trusted him. Alcohol blurred everything, and I blamed myself. That trauma left deep scars—anxiety, panic attacks, sleep problems, an eating disorder, and constant hypervigilance.
In October 2014, my pain attacks became overwhelming. I didn’t know why, but I couldn’t cope anymore. A year later, I received my CRPS diagnosis. My physical and mental struggles reshaped my entire life. I now have more medical appointments than visits with friends.
Over six years, I endured continuous pain treatments, yearly surgeries, medication changes, injections, and ketamine infusions. None of them work perfectly, but they help me survive one day at a time. Ketamine, while necessary, often causes terrifying dissociation and loss of reality. Around this time, I was also diagnosed with Borderline Personality Disorder, likely rooted in adolescence. I wore a mask, smiled through pain, and felt empty inside. I began self-harming as a way to cope with fear, stress, guilt, and pain. Eventually, this led to suicide attempts and escalating self-harm.
In 2020, I experienced sexual abuse again—this time by a friend I had known for three years. The manipulation left me ashamed and broken. I struggle to cry, holding everything in until it overwhelms me. I self-harm to manage guilt and redirect pain because the chronic pain feels unbearable. Self-harm is not about attention—it is about survival. Every scar has a story.

I started my Instagram account to share my truth, connect with others, and remind people they are not alone. It became a place for honesty, positivity, and small moments of beauty. Nature helps me heal, even if only briefly, and photography allows me to share that part of my life too.

Things may be incredibly hard—but they are not impossible. Let go of what you cannot control, and focus on the moment you are in right now.