I started getting migraines when I was 26. Both my father and sister had a history of them, so at first, I didn’t think much of it—it just seemed like it was “my turn.” I asked friends and colleagues for advice, tried every remedy I could find, and slowly came to the resigned belief that migraines were just going to be a part of my life.

But then my migraines started to change. I was a Ph.D. student at the time, working on campus as usual, when I noticed the familiar small blurry spot in my left visual field. Normally, it would expand slightly before fading, but this time, the blur spread rapidly until I couldn’t see anything at all. Then, as if that weren’t alarming enough, the left side of my face went numb—my left arm followed. I somehow made my way to the campus health center, probably walking crookedly on account of my blurred vision. I explained my symptoms to the physician and, to my disbelief, was sent home with the suggestion to take Tylenol.
Later that year, the migraines worsened. Nighttime acid reflux became frequent, and numbness in my left hand started to occur more often. I repeatedly called my neurologist’s office, hoping for an earlier appointment, but there were none. Then came the symptom that finally sparked real fear: dizzy spells. What we would later learn were focal seizures. They struck randomly—while I was walking, typing for long stretches, or even in the middle of the night. I would feel faint, go to the ground, and press my head to the floor. When they ended, acid would rise in my throat, leaving me confused and anxious. For a brief, absurd moment, I even wondered if I could be pregnant.

After enduring these seizures for nearly a month, I finally called the neurologist’s office again. I described everything and, after multiple calls, secured a video appointment. The doctor conducted a thorough neuro evaluation, repeated the usual information about migraines, and scheduled an MRI for the first available slot later that month.
The day of the MRI was rainy and gloomy, and I almost didn’t go. But then I thought it would be kind of fun to have brain images to show my students when teaching an Intro Psych class on brain imaging. Curiosity and the promise of quirky PowerPoint slides pushed me forward. I got the MRI, stopped by Target on the way home, and prepared for the week ahead.
That night, around 10:30 p.m., my phone rang. At first, I ignored it, thinking it was strange. Then I noticed the hospital’s area code and decided to check the voicemail. What I heard shattered my world. The doctor’s message was simple but devastating: get to an emergency room immediately and page him. I fell to the floor. My husband helped me up, and we called the doctor.
“There is a large mass in the right hemisphere of your brain.”
We called my parents, packed a bag, and prepared to leave. On the way, I paused in the bathroom, looking at the mirror and crying. I had a habit of writing goals on sticky notes and posting them on the mirror. One note held a pregnancy test I had marked with a red Sharpie as a hopeful reminder for the future. That night, I cried—not for the missed possibility, but for the remarkable way my body had been signaling the timing all along.
We drove to the emergency room. My husband remained calm, my rock as my world tilted. Because of COVID, he couldn’t accompany me inside, and my parents met us later. I walked into the ER—the scariest place I could imagine—alone but steady.
I looked down at my left wrist, at my “Still I Rise” tattoo. I had gotten it after my first year of teaching, thinking nothing could challenge me more than that experience. In that waiting room, it reminded me of my students and gave me strength.
Once called back, I was hooked up to monitors, and a PA explained the MRI findings. The mass was large. I called my mom, dad, and husband so they could hear it from me. My mom asked if I would send her a picture of the MRI. I hesitated, then said, “Are you sure? It’s big.”

Then, unexpectedly, I laughed. The PA looked confused, and I explained, “I just know way too much about this.” We laughed together, and soon I was admitted to neurosurgery. My assigned neurosurgeon reviewed my MRI, explained the probable diagnosis, and outlined the plan. The first step: surgery to remove as much of the tumor as possible. Surgery would be scheduled soon, but not immediately. I was discharged with anti-seizure medication, a fear I had never known, and a strange, comforting sense of safety from my incredible medical team.
The month before surgery stretched both quickly and painfully slow. Doctors called the tumor “most likely a glioma,” and I avoided Googling the term. One article, sent by someone, confirmed my worst fears, and I cried for days before focusing back on the upcoming operation. At one point, I nervously asked a nurse about being awake during surgery. He teased, “You’ve been watching too much Grey’s Anatomy, haven’t you?” But yes, I was scheduled for an awake craniotomy.
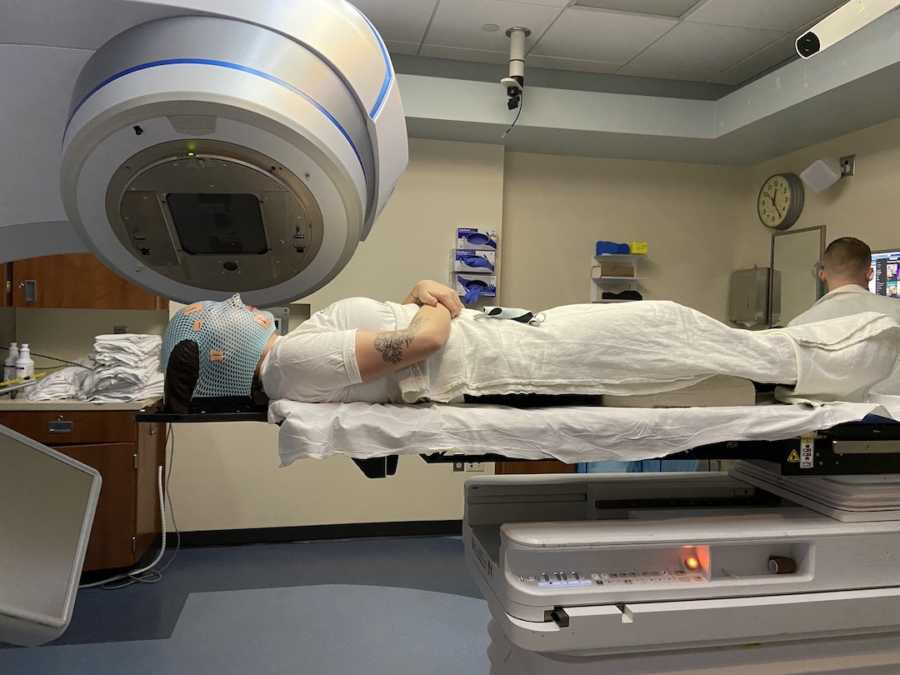
In the days leading up to surgery, adrenaline, reading, and hours of The Office filled my time. The night before, my neurosurgeon called. “Are you ready?” I asked. “I’m ready,” he said. I went to sleep surrounded by family, surprisingly calm.
Surgery day arrived. Pre-op introductions, safety checks, and a flurry of professionals surrounded me. I remember waking briefly, feeling cold, a nurse giving me a blanket, another placing a wet sponge in my mouth, and answering questions during the awake portion. And then, waking in the post-op area, I saw my mom, my nurses, my surgeon, and thought, Thank you, thank you, thank you.

I spent four days in the ICU, two on the Neuro floor. Sleep, neuro checks, and the kindness of healthcare workers filled those days. I took videos, went live on Instagram, and marveled at my recovery. Post-surgery MRI results were beyond what we expected. I walked for the first time, ate my first proper meal, and went home exactly a week after surgery.
Returning home felt strange. I had to relearn to trust my body. My mom helped me shower, my dad made breakfast, my husband guided my steps, and my dog cuddled with me through it all. Pain management was intense: headache wraps, oversized sunglasses, pillow towers, and nightly mantras: “I am healthy, I am well, I feel good, I feel swell.”

Weeks later, appointments resumed. Pathology confirmed an anaplastic astrocytoma, grade 3, IDH mutant. Treatment was planned: chemotherapy and radiation. At first, the idea of “fighting” felt wrong—I didn’t want to fight my brain, only to love it, to care for it, to honor it. Fertility preservation was planned, new doctors joined my team, and I learned the rhythm of treatment: daily radiation, daily chemo, blood tests, MRIs.

Through it all, I hope readers understand: you don’t need to fight your body. You can love it, even in the unimaginable. You can kiss your brain, thank it for all it does, and hold hope through the darkest moments. And if you can, do it now—kiss your brain, whisper gratitude, and remember how remarkable you truly are.