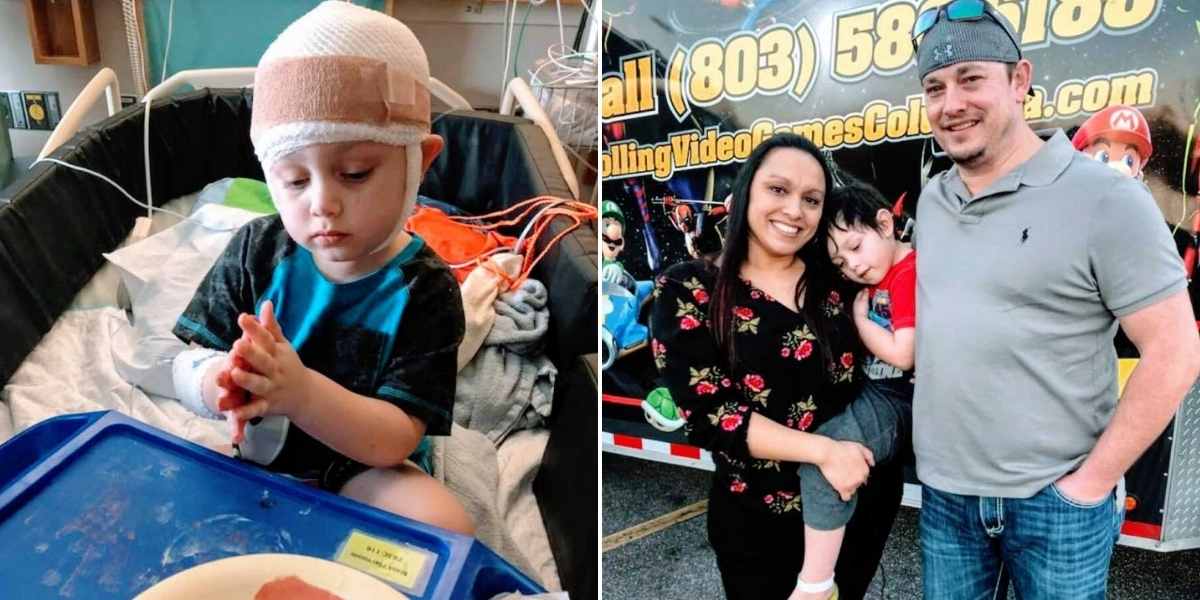
It’s the kind of moment no parent ever prepares for, one you never expect to arrive overnight—but every parent of a special needs child knows the feeling. In the summer of 2016, my son Cayden had his very first seizure. He was just over two years old. That first seizure is etched into my memory forever. I was watering our tomato garden, and since Cayden had been sick, he was outside in just his diaper, happily sucking on a lollipop while the cool mist from the hose sprayed us. I thought it might help with his fever. Out of the corner of my eye, I saw him fall, and his lollipop tumbled to the ground. “Oh honey, it’s okay, Mama’s got it,” I said, reaching to help—but then I realized he had flopped backward and was convulsing.
I dropped the hose and scooped him up, running to the front yard while shouting to neighbors to call 911. I held my two-year-old as his little body shook uncontrollably, his eyes rolling back. Time felt like hours, though it was only minutes, and I found myself praying aloud, begging God to protect him. When the ambulance arrived, I handed him to his Godmother to grab clothes, my phone, and essentials. The ride to the hospital was a blur. They monitored him, and once he woke, everything seemed normal, so we were sent home with instructions to follow up with his pediatrician. For weeks afterward, fear kept me from sleeping, haunted by the thought of it happening again. His doctor reassured us it was a febrile seizure—common when children spike a fever—and we tried to return to normal life. Cayden went back to preschool and everything seemed fine.

Almost exactly a year later, just before summer, Cayden got sick while visiting friends. A fever rose, and another seizure struck. Again, the hospital observed him, released us, and his pediatrician still believed it was just febrile seizures. Life went on. We celebrated family, prepped for school, and watched Cayden thrive at preschool—bright, sweet, and excelling in every way. Then came the seizure without a fever, this time at school. My gut screamed that something was wrong. His pediatrician agreed and referred us to a neurologist. At the time, my marriage was falling apart, yet we focused on Cayden, scheduling an appointment a month away.
The first office visit included a brief EEG with the PA neurologist, who was kind and attentive. He recommended an emergency seizure medication and trained me on its use. About a week later, Cayden had another seizure. EMTs questioned why he wasn’t on a regular anti-seizure medication, and I started asking myself the same thing. We scheduled a follow-up; the neurologist agreed to an overnight EEG to better understand his seizures. Just a week before the procedure, Cayden seized at home again.

The overnight EEG at the hospital was our chance for answers. The neurologist on duty was the epilepsy specialist, normally too busy to meet us. Cayden was cooperative as they hooked him up to video monitoring and conducted blood and urine tests. The next morning, the doctor bluntly confirmed it: Cayden had epilepsy. His bedside manner was awful, but the message was clear. With four seizures already, it was time to start anti-epileptic drugs. We began Trileptal, a sodium channel blocker, hoping it would stop the misfires in his brain.

Cayden’s dad and I had different approaches—he trusted the doctors, I needed concrete answers before giving him medications that scared me. As fall turned to winter, I noticed dramatic changes in Cayden. My once-happy, carefree child became withdrawn, avoiding play with siblings and classmates. Any parent of a special needs child knows that sinking feeling—helpless, watching your child change before your eyes. I called the doctor, but he dismissed it as side effects. Weeks before Christmas, another seizure struck. We increased the medication slightly, hoping it would help. Christmas in California was bittersweet as I prayed for Cayden’s safety.

By January, Cayden was having breakthrough seizures, five by mid-month, despite his medications. I demanded hospitalization. The neurologist admitted the medicine wasn’t working and switched him to Keppra, a calcium channel blocker. Two days later, we went home, but I felt broken and frustrated—the hospital seemed powerless to truly help my son. Days blurred as Cayden started each morning with a seizure. I returned to the ER, begging for solutions, but was repeatedly told to adjust medications.

Finally, a breakthrough came on January 26th. The PA neurologist consulted Dr. Anna Mrelashvili, who immediately recognized the danger. We were admitted, and from our first conversation, I knew she was listening and committed to finding answers. Cayden underwent 24-hour EEG monitoring. Seizures continued, he declined rapidly, and my gut ached with each one. Nurses like Molly became our lifeline, caring for him with patience and warmth. On February 4th, after back-to-back seizures, he was moved to the PICU. Dr. Anna adjusted medications, switching him to Depakote and adding Onfi. Other doctors disagreed, but Dr. Anna’s judgment was the only one I trusted.

Cayden required in-patient rehabilitation for walking and speech. At Atlanta Children’s Hospital, he relearned skills he had lost. Though he returned home to a new normal—wheelchair use, medications, helmets—the love and laughter in our household persisted. Yet just a week later, a breakthrough seizure struck during a car ride. Status epilepticus followed, and we were rushed back to the PICU. The on-call neurologist admitted Cayden’s case was beyond their experience. We waited anxiously for Dr. Anna, our lifeline, to arrive and guide us toward stabilization.
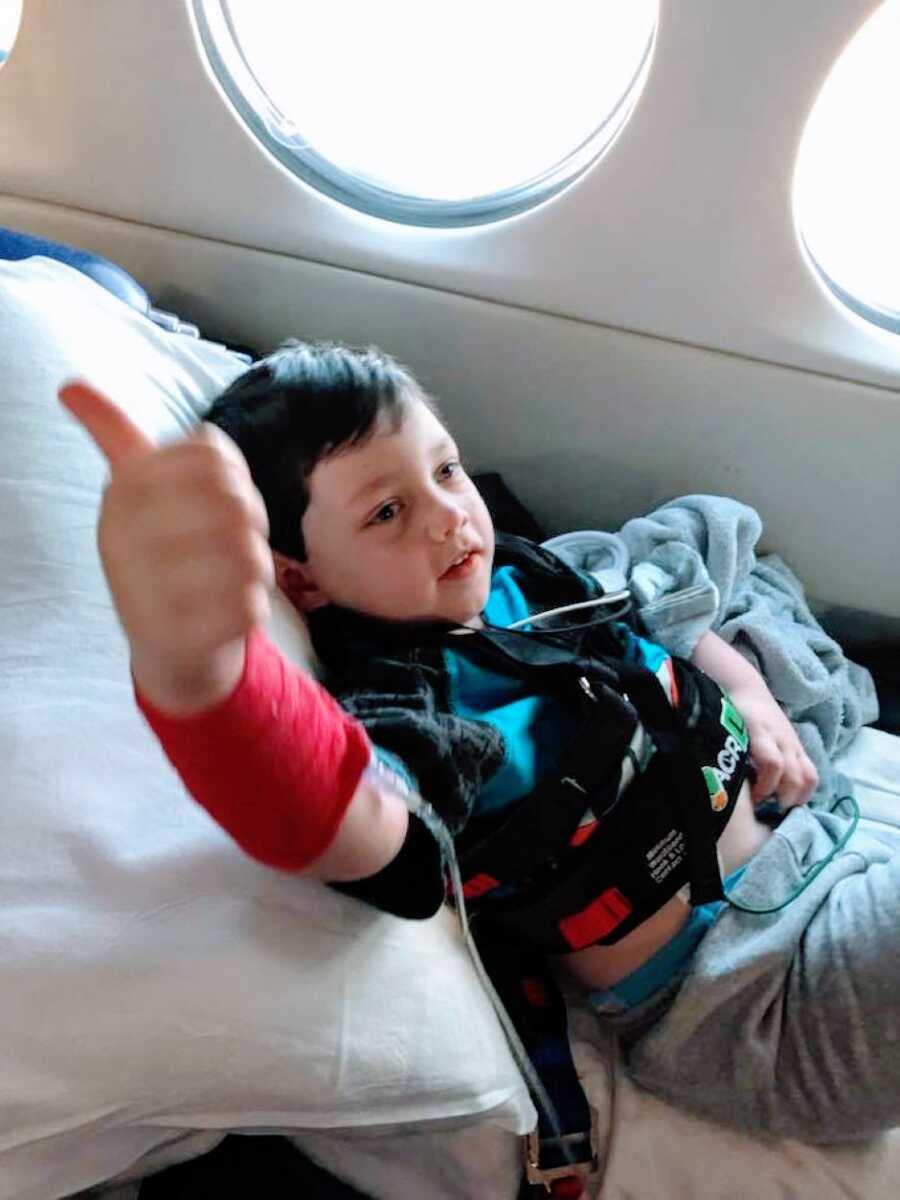
Eventually, we transferred to the Mayo Clinic, hoping brain surgery might cure him. Cayden endured two days of seizures without medication to test candidacy. They discovered a brain malformation and ruled out surgery. Vimpat worsened his condition; the keto diet was impractical for a three-year-old. Finally, Le Bonheur Children’s Hospital took him. Under Dr. Wheeles and his team, Cayden’s medications were adjusted, and three days later, he was seizure-free. Progress was rapid—coordination and speech improved daily. After two weeks, we returned home, embracing a life that felt foreign yet precious.

While our family faced challenges—my marriage didn’t survive, my other children endured immense stress—Cayden’s recovery was a blessing. He now thrives: playful, witty, loving, and curious, with a passion for trains, Minecraft, and PJ Masks. He takes five daily medications to stay safe, but his joy, humor, and love for life are intact. Our journey isn’t over, but we are grateful—Cayden is home, thriving, and showing us the incredible resilience of a child and the power of unwavering parental love.